It’s the right decision for now
I’ve been a volunteer coach with the Sports Backers Marathon Training Team for 5 years. That’s 6 months of each year dedicated to helping my Richmond running community meet their running goals.
2022 was a tough year for my family. 2023 wasn’t much better. And for my mental health, I need to take time and space for myself so that I can be more dedicated to my recovery and my family.
This was a tough decision that I did not take lightly. I could make arguments both for continuing and stepping back. But in the end, I realize that I can’t pour from an empty cup.
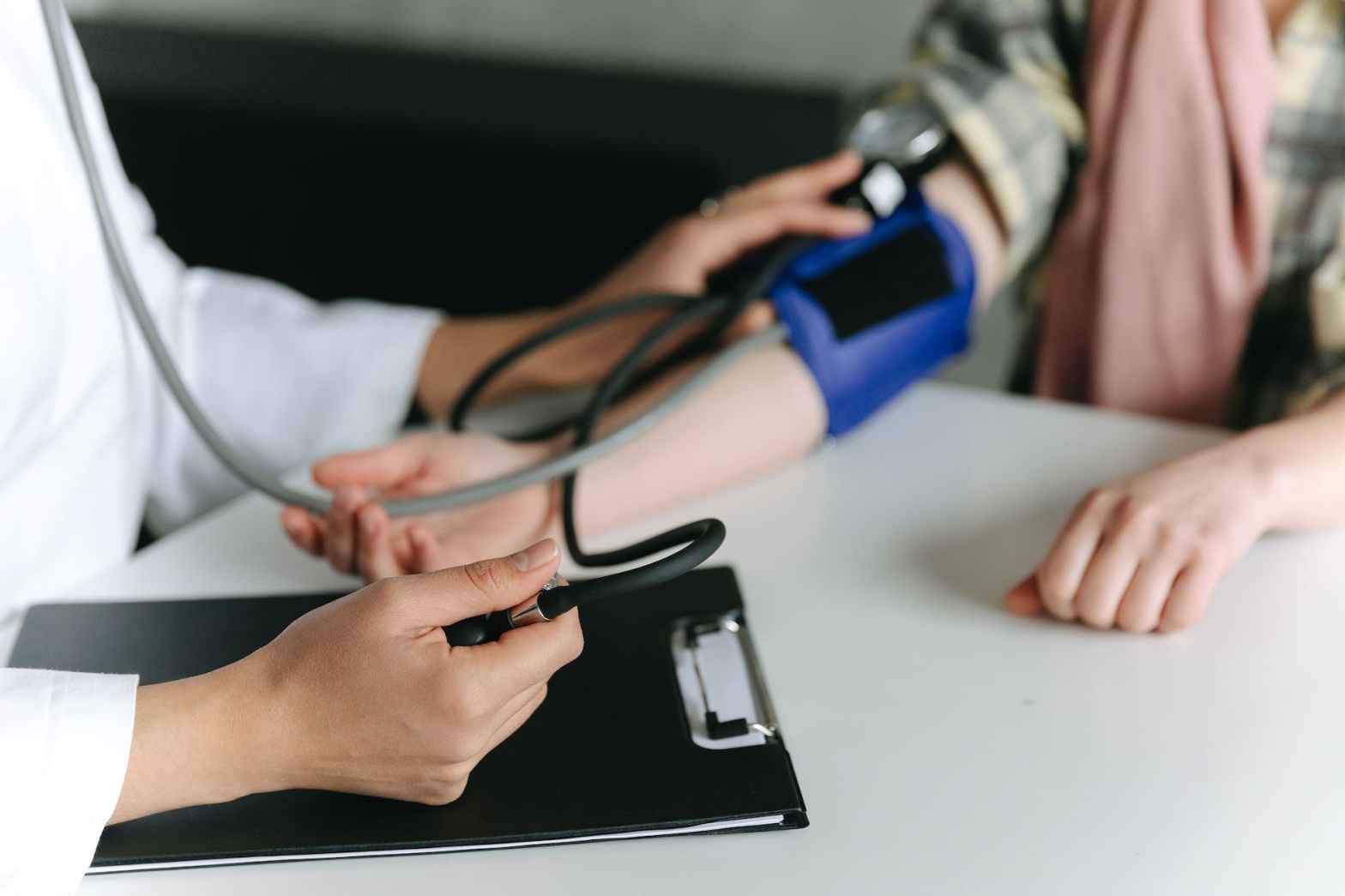
Following the shooting, my life simply hasn’t been the same. I lost my entire fall season to rehab. I still suffer from frequent headaches due to significant hypertensive episodes. I am on three new medications to manage my blood pressure and to help me sleep. My nights are still plagued by insomnia and nightmares without the sleep aid.

I have no reason for my new diagnosis of hypertension except for anxiety. And while I may not outwardly feel anxious, my body says otherwise. I am not obese. I am a marathon runner. My cholesterol is 160. I’m vegan. My resting heart rate is 51. My heart rate alone makes my blood pressure difficult to control, as an entire class of drugs has to be eliminated from the choices to manage this (beta blockers).
My blood pressure and the side effects of all of my new medications have kept me from running lately. My body is still trying to adjust.
It’s frustrating because I relied on exercise so much to manage stress, and now it seems it’s not an option. Not only is it suddenly physically challenging, but I’m also trying to figure out how harmful my running habit is, as my therapists tried to convince me that running is a process addiction for me. Maybe they just don’t understand the mentality of a marathon runner.
The fact is that post-rehab, I’m tired all of the time.
On days that I work, I come home and take at least an hour-long nap. Some days, that nap is more like 3 hours. Granted, as a hospital-based physical therapist, my job is physically, mentally, and emotionally challenging. By the end of my work day and despite medication, my blood pressure will creep up to dangerous levels due to all of the demands on my body. I may have to help transfer a dependent patient by using my muscle power to lift them out of bed. I also have to be focused enough to make good clinical decisions as well as provide emotional support to those I serve.
I used to have space for all of these demands, plus running and taking care of my family. Those days seem over now. I’m grieving this loss that wasn’t my choice. It was imposed upon me.
I used to take pride in my mental toughness. Despite all of my childhood trauma, I managed to have a pretty successful life. I graduated college magna cum laude. I went on to my top choice for PT school, passing my boards on the first attempt. I got married. I have two amazing daughters. I am a 10-time marathon finisher and ultrarunner. And I am heavily involved in my Richmond running community.
But the shooting broke me. It’s hard to admit, but it has. I’m not the same person I was before the event.
It doesn’t help that I can’t escape the scene of the crime. I think that was the most valuable part of going to inpatient treatment following the acute trauma; that I could escape the place where it happened. But now that I’m back, I’m struggling more than I anticipated.

It’s not as simple as moving. My husband and I built this house as our forever home. We built on his parents’ land, and we live next door to them. We need to stay here to help care for my mother-in-law.
I love my home, but there is a part of me that will never fully feel safe here again. And that is sad and challenging for me.
The financial burden of treatment, transportation to get there, and loss of my salary are significant. We also had difficulty finding a lawyer willing to take my case to recover financially because I didn’t suffer a physical injury.
Some days, I wish the bullet had struck me. The damage would have been easier to prove and for others to understand.
With all of the progress we seem to have made as a society in reducing the stigma attached to mental health issues, the line gets drawn here. Legally, it seems that it is still some kind of moral failure on my part that my brain couldn’t handle the stress of feeling like it was being hunted.
And while the 21-year-old men who are responsible for the damage to our home and mental health got by with merely a slap on the wrist, my life, and the lives of my family, are irreparably harmed.
Giving up coaching is one of the toughest choices I have made, as it was so much a part of my identity. I will be grieving this loss for a while.
___________
The lead photo shows my fellow coaches and me at the finish line of the Richmond Marathon in 2021. Photo from author’s archives.
As always, I hope you all are safe and healthy.